BACK TO RESEARCH WITH IMPACT: FNR HIGHLIGHTS
An estimated 55 million people in the world suffer from dementia, with the number estimated to increase to 78 million by 2030. In Luxembourg, more than 10,000 people suffer from dementia, including patients affected by Alzheimer’s disease and Dementia with Lewy Bodies. These incurable diseases have an increasing socio-economic impact along with the burden on patients and caregivers. One of the approaches researchers are taking is studying microglia, immune cells in the brain.
“The terrorist inside my husband’s brain” is the title of an editorial written by the wife of comedian Robin Williams after the actor’s suicide in 2014[1]. Next to Rita Hayworth, Robin Williams was perhaps the most known patient suffering from Dementia with Lewy Bodies, known as DLB. According to William’s wife, the havoc DLB was wreaking played a large part in the deterioration of the actor’s mental health and subsequent suicide.
Alzheimer’s disease (AD) and Dementia with Lewy Bodies (DLB) all revolve around neurodegeneration, which involves a serious loss of neurons.
“After a long phase without symptoms, patients suffer from an irreversible and unstoppable decrease of cognitive functions, including memory decline and loss – i.e., dementia. Whereas the motor symptoms of DLB patients can partially be alleviated, and despite a recently FDA-approved drug for AD, no treatment to cure neurodegeneration-related dementia is available,” explains neuroscientist Sonja Fixemer.

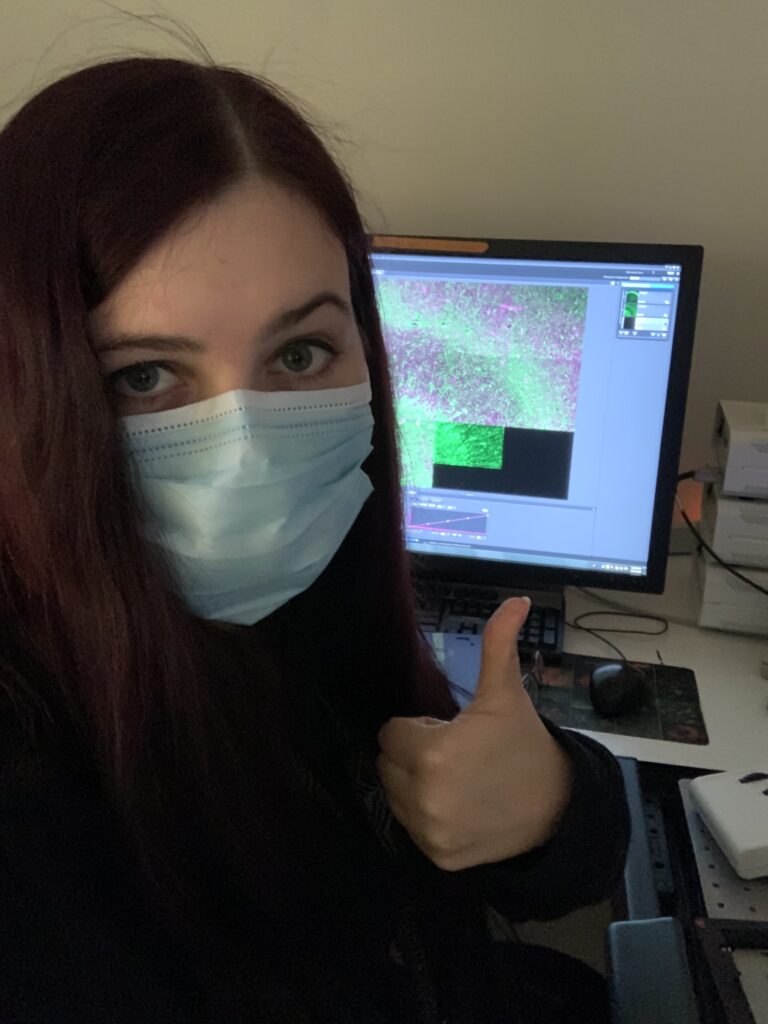
This image shows that many of the brain’s immune cells, called microglia (in magenta) have ‘ingested’ some of the disease-typic accumulations of misfolded protein amyloid beta (in green). As immune cells they try to get rid of the toxic accumulations, but it seems that factors such as disease chronicity drive the cells in a state of exhaustion or overreaction and therefore might actively contribute to neurodegeneration.
(3D high-resolution confocal image, magnification 93x)”
The search for a cure
As with many diseases tied to ageing, AD and DLB are on the rise, and along with it the burden on patients’ and caregivers’ quality of life, not to mention the socio-economic impact. Science still searches for a cure, and answers to questions about how these diseases come to be.
“In most cases AD and DLB appear in a sporadic manner, meaning that there is no known genetic component, and the causes remain unknown,” Sonja explains.
“On the neuropathological level AD and DLB are characterised by disease-typical aggregations of toxic proteins, namely amyloid-beta plaques and neurofibrillary tangles[2] in AD and Lewy bodies and Lewy neurites[3] in DLB.
“In fact, these toxic proteins often appear in a mixed manner between both diseases. Although many therapies are targeting these toxic protein aggregations, none have so far showed the desired effect to stop or reverse the disease.”
Microglia – a possible target for treatment
A target researchers have recently set their focus on are the resident immune cells of the brain – microglia, representing 5-8% of all brain cells. Evenly distributed throughout the brain, microglia continuously survey the tissue with the aim of detecting and clearing pathogens and cell debris. They also have a direct line of contact with other cell types of the brain, to ensure the proper functioning of the central nervous system.
“Upon post-mortem analysis of the brains from AD patients, microglia were shown to change their shape and re-organise their distribution. A more recent hypothesis is that microglia are not a homogenous cell population but can be divided in several functionally diverse subpopulations that could react differently upon disease impact. However, if, which and how subpopulations remain protective or even contribute to disease progression, is still unclear,” Sonja explains.

Neuroscientist Sonja studies alterations in microglia, in the context of mixed toxic protein aggregations. This is done by analysing post-mortem brain tissue from AD and DLB patients, as well as age-matched control subjects.
“We conduct our study on a brain region called hippocampus, which is central in memory processes, however its subregions are differently affected by neurodegeneration in AD and DLB patients.”
“Across three hippocampal subregions, we analyse the precise amyloid-beta, tau and phospho-alpha-synuclein burdens in each patient and investigate how microglia react to this complex neuropathological context composed by various toxic protein accumulations.”


Photos by Sonja Fixemer
Sonja & team have discovered that altered microglia morphologies are associated with a precise mix of toxic protein burdens. This effect is particularly strong in a hippocampal subregion that is more severely affected by neurodegeneration in AD patients, compared to DLB patients. This observation suggests that microglia could be targeted for new therapeutic treatments in both diseases, but especially in AD.[4]
Comfortable with the science language in this topic? Read more below in our ‘peer to peer section’
Sonja Fixemer is a 4th year PhD candidate in the Integrative Cell Signalling Group, led by Prof Alexander Skupin (Luxembourg Centre for Systems Biomedicine (LCSB) at the University of Luxembourg), and is also tied to the Luxembourg Centre for Neuropathology (LCNP), led by FNR PEARL Chair Prof Michel Mittelbronn. Her project is part of the FNR PRIDE Doctoral Training Unit (DTU) Park-QC. Sonja’s research is supervised by Dr David Bouvier.


[1] https://n.neurology.org/content/neurology/87/13/1308.full.pdf
[2] composed of phospho-tau protein
[3] composed of phospho-alpha-synuclein protein
[4] https://actaneurocomms.biomedcentral.com/articles/10.1186/s40478-022-01342-7

RELATED FUNDING

MORE ABOUT SONJA FIXEMER
On her research peer-to-peer
Milestones in the project
“In our recently published paper4 we describe how microglia phenotypes are associated with subregional patterns of concomitant amyloid-beta, tau and phospho-alpha-synuclein pathologies in the hippocampus of patients with AD and DLB. For example, the higher the combined burdens of phospho-tau and phospho-alpha-synuclein are, the more severe microglia morphologies are altered. This effect is most pronounced in AD patients in the hippocampal subregion CA1, which is particularly vulnerable for atrophy in AD. The impact is less severe in hippocampi of DLB patients but follows a similar trend. This suggests that microglia alterations associated to high phospho-tau and phospho-alpha-synuclein could be a factor in CA1 vulnerability in AD. This also implies that microglia could be targeted for new therapeutic treatments in both diseases, but especially in AD.”
Methodology
“We used confocal fluorescent microscopy of immunostained brain sections from 29 individuals, to obtain 3D images of amyloid-beta, phospho-tau and phospho-alpha-synuclein burdens, as well as microglia morphologies. This means we acquired 348 high-content images, which represent more than 500GB of data after processing. We performed volumetric analyses of the three toxic protein burdens using AI-assisted image analysis tools; and analyzed more than 32,000 3D microglia morphologies based on 16 morphological features using our in-house developed pipeline called MIC-MAC.
We identified two distinct microglia clusters enriched in disease conditions and particularly increased in CA1 and DG/CA4 of AD and CA3 of DLB patients. Our study confirms frequent concomitance of phospho-tau, amyloid-beta and phospho-alpha-synuclein loads across AD and DLB but reveals a specific subregional pattern for each type of pathology, along with a generally increased severity in AD. Furthermore, phospho-tau and phospho-alpha-synuclein loads were highly correlated across subregions and conditions. We uncovered tight associations between microglial changes and the subfield pathological imprint. Our findings suggest that combinations and severity of subregional phospho-tau, amyloid-beta and phospho-alpha-synuclein pathologies transform local microglia phenotypic composition in the hippocampus.”
On her fascination for immunology and neuroscience
“Already as a child I had a curious nature and was fascinated by life sciences in general. During my university studies I got particularly hooked on the fields of immunology and neuroscience: it is just incredible how the immensely complex immune and nervous systems are orchestrated and can react in a very precise manner. And at the same time, how a disbalance in these systems can produce devastating diseases. This led me to pursue my PhD studies in the field of neuroimmunology.”
On where she sees herself in 5 years
“After finishing my PhD, I plan to continue my studies as a Post-doc on a similar topic involving glia cells, which are still underestimated components of the brain and essential for proper functioning of the nervous system.”
On returning home to Luxembourg for her PhD
“I am originally from Luxembourg and after spending almost 5 years in Strasbourg, France, for my Bachelor and Master studies, I was pleased to return home for the PhD adventure with my family and friends nearby.”
Sonja has taken part both in the Science Festival, as well as two editions of Chercheurs à l’école, where researchers go back to school. Sonja, why do you feel it is important to connect with the general public and school students? (what do you enjoy about these outings, why are they important?)
“To me it is always a great pleasure to share my passion about science and research to the general public or school students. It is a great opportunity to provide some insights on biology and research and at the same time try to spark interest in these topics. I can only recommend to other researchers to take part in such outreach activities, because it is truely stimulating to discuss with the lay audience as it also allows us to see our research topics from a broader point of view, compared to the typically very detailed technical discussions with other expert scientists.”
About Spotlight on Young Researchers
Spotlight on Young Researchers is an annual FNR campaign where we shine a Spotlight on early-career researchers across the world with a connection to Luxembourg. Nearly 100 features have been published since the first edition in 2016.
Browse them below!